Understanding Uterine Fibroids
Evidence-based, professional, and accessible information about uterine fibroids to help every woman make informed health decisions.
peak prevalence at age 45-49
Chinese population study
of reproductive-age women affected
extremely low malignancy risk
Understanding Uterine Fibroids
Learn about the most common benign tumor in women
Uterine fibroids (also called leiomyomas or myomas) are benign tumors that develop from the smooth muscle tissue of the uterus. They are the most common benign tumors in women. They are NOT cancer and rarely become malignant. Understanding them is the first step to overcoming fear.
What Are Uterine Fibroids?
Uterine fibroids are benign tumors formed by abnormal proliferation of uterine smooth muscle cells. They can be single or multiple, ranging from a few millimeters to over ten centimeters. Fibroids are hormone-dependent — their incidence increases with age during reproductive years and they tend to shrink after menopause.
How Common Are They?
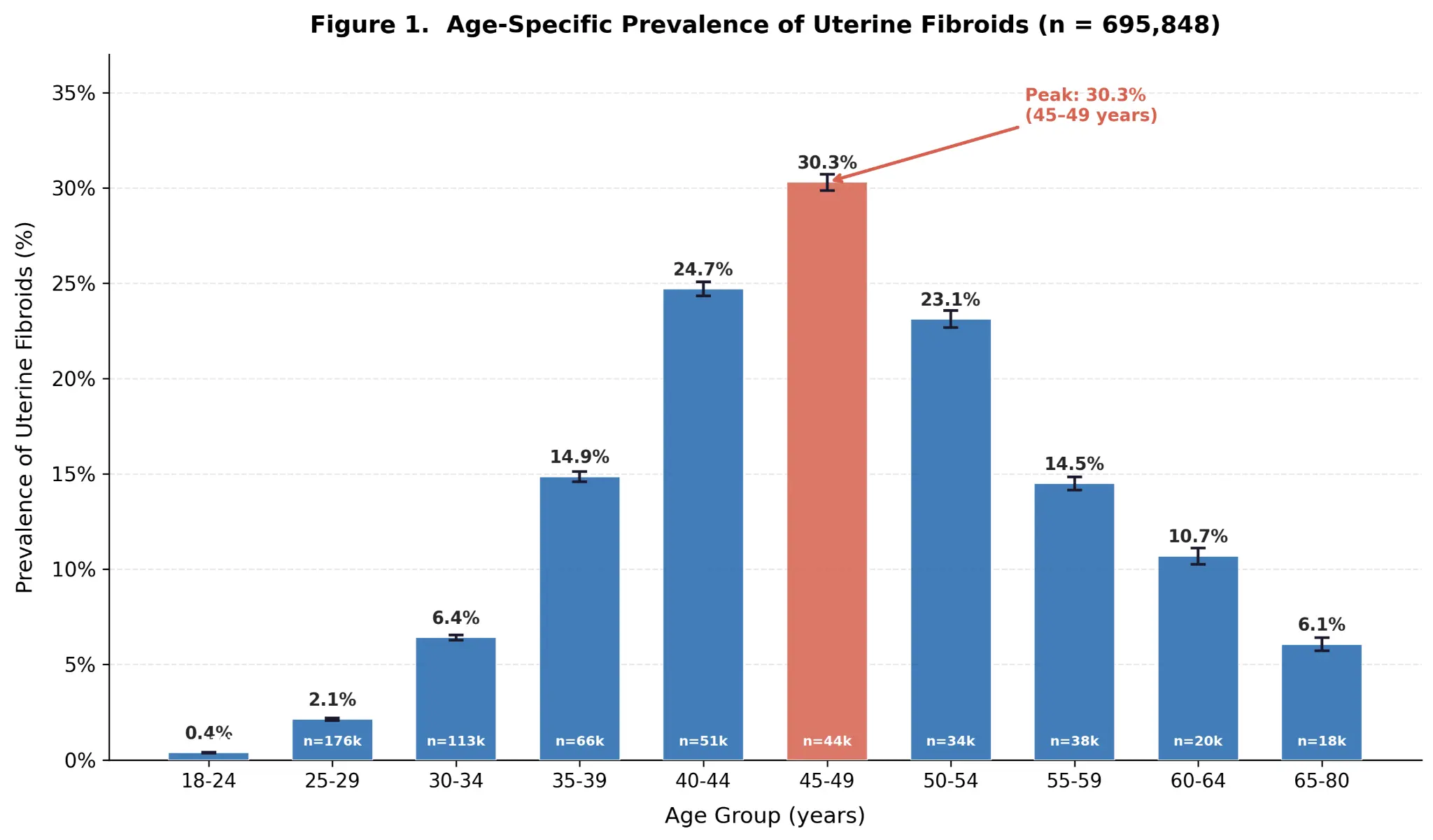
According to a large-scale epidemiological study of nearly 700,000 Chinese women by the Woyi team, fibroid prevalence varies significantly with age: only 0.4% at ages 18-24, 6.4% at 30-34, 24.7% at 40-44, peaking at 30.3% at ages 45-49, then gradually declining. Overall, approximately 25% of reproductive-age women are affected — roughly 1 in 3-4 women.
Chinese 700K Population Study
Woyi Team Research Data (n=695,848)
Based on a cross-sectional study of 695,848 Chinese women, the Woyi team systematically revealed the age-specific prevalence distribution of uterine fibroids in Chinese women for the first time. The study found prevalence peaks at 30.3% in the 45-49 age group, providing important epidemiological evidence for clinical decision-making.
Types of Fibroids
Based on their relationship to the uterine wall, fibroids are classified into three main types:
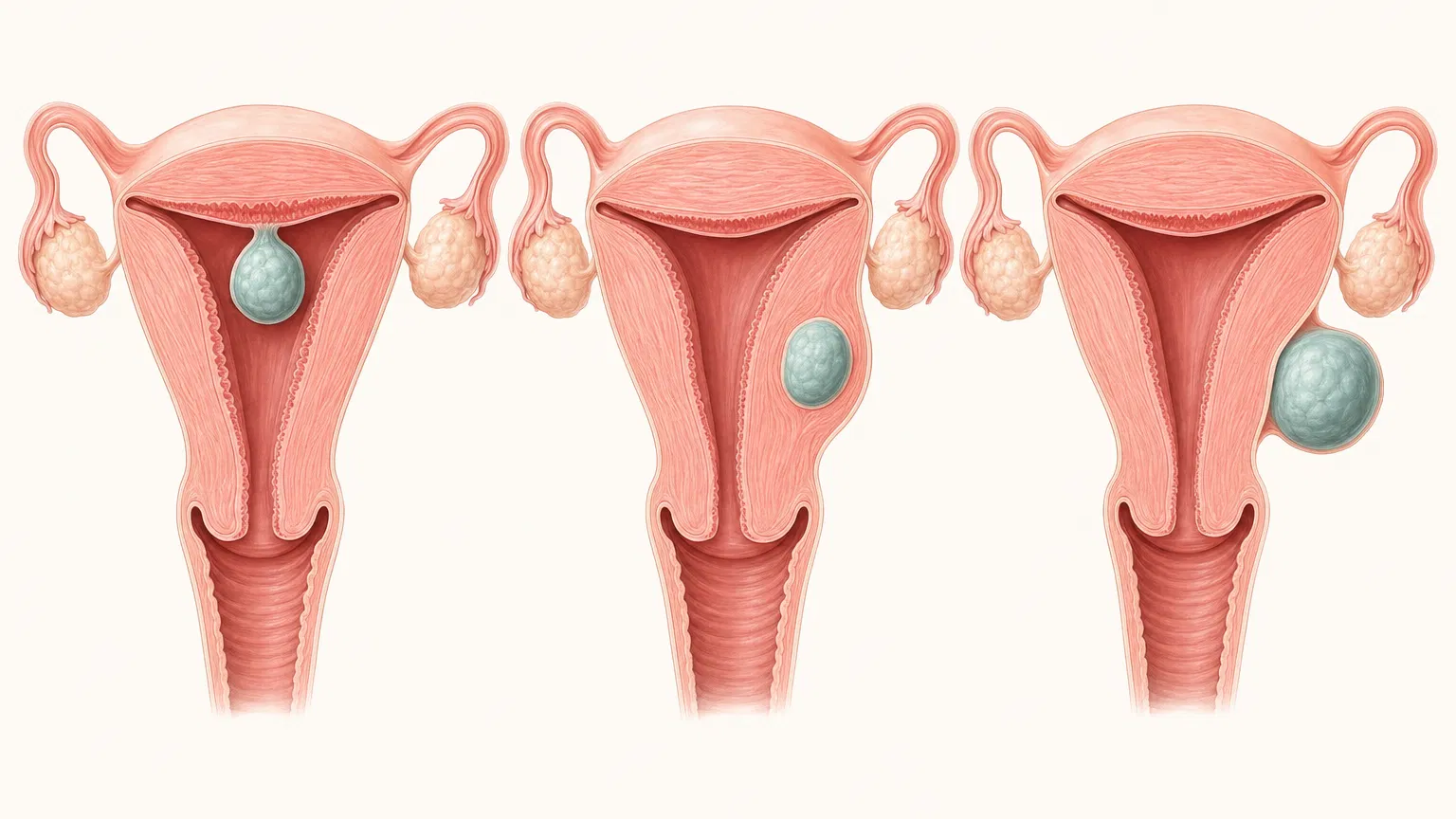
Submucosal Fibroids
Grow into the uterine cavity. Even small ones can cause heavy menstrual bleeding and irregular periods. Correspond to FIGO types 0, 1, and 2.
Intramural Fibroids
Located within the uterine wall and are the most common type. When enlarged, they may distort the uterine cavity or serosal surface. Correspond to FIGO types 3, 4, and 5.
Subserosal Fibroids
Grow outward from the uterine surface. Usually cause milder symptoms but may compress surrounding organs when large. Correspond to FIGO types 5, 6, and 7.
FIGO Classification System
The International Federation of Gynecology and Obstetrics (FIGO) classifies fibroids into types 0-8 based on location, helping doctors precisely describe fibroid position and guide treatment decisions.
Symptoms & Signs
Understanding the potential impact of uterine fibroids
About 70%-75% of women with fibroids have no noticeable symptoms and are often discovered incidentally during routine examinations. When symptoms occur, they are mainly related to the size, number, and location of fibroids.
Abnormal Uterine Bleeding
The most common symptom, presenting as heavy menstrual bleeding, prolonged periods, or intermenstrual bleeding. Submucosal fibroids are particularly prone to causing bleeding, which may lead to anemia over time.
Pain & Discomfort
May include worsening menstrual cramps, lower abdominal heaviness, and lower back pain. Fibroid degeneration (such as red degeneration) may cause acute pain, but this is generally not a cause for excessive concern.
Pressure Symptoms
Large fibroids may compress the bladder causing frequent urination, compress the rectum causing constipation, or compress the ureters potentially causing hydronephrosis.
Fertility Impact
Some fibroids may affect conception or increase miscarriage risk, especially submucosal and large intramural fibroids. However, many women with fibroids can still conceive and deliver normally.
Other Symptoms
Some patients may experience abdominal mass sensation or discomfort during intercourse. Chronic anemia from prolonged heavy bleeding may cause fatigue, dizziness, and palpitations.
Asymptomatic Fibroids
Most fibroids are asymptomatic and do not require treatment. Evidence-based medicine shows that fibroids without symptoms, even if larger than 5cm, do not necessarily require surgery. No international guideline has ever listed fibroid size as the sole surgical indication.
When to See a Doctor?
Seek medical attention when experiencing significantly heavier periods, periods lasting more than 7 days, intermenstrual bleeding, severe anemia, significant pressure symptoms, or acute abdominal pain.
Treatment Options
Individualized treatment choices
Treatment of uterine fibroids should be individualized, considering the patient's symptoms, age, fertility desires, and fibroid characteristics. Evidence-based medicine emphasizes: treatment should only be considered when benefits outweigh risks.
Watchful Waiting
AFor asymptomatic or mildly symptomatic fibroids, watchful waiting is the preferred strategy recommended by international guidelines. Fibroids are hormone-dependent and naturally shrink after menopause. No international guideline has ever listed fibroid size >5cm as a surgical indication — symptoms are what matter. Regular ultrasound follow-up every 6-12 months is sufficient.
Evidence-Based Treatment Principles
Whether non-invasive, minimally invasive, or open surgery, all procedures carry potential risks for patients. Treatment should only be considered when benefits outweigh risks. Surgery should not be the first choice — minimally invasive ablation therapy is an excellent alternative.

Professional Treatment Center
Woyi Uterine Fibroid Minimally Invasive Treatment Center
The Woyi Uterine Fibroid Minimally Invasive Treatment Center is dedicated to providing professional, minimally invasive, and individualized care for fibroid patients. The center brings together experienced gynecological specialists using internationally advanced minimally invasive techniques to help patients achieve optimal outcomes with minimal trauma.
Clicking will redirect to the official Woyi website
Woyi Uterine Fibroid Minimally Invasive Treatment Center
www.woyigroup.com
Frequently Asked Questions
Evidence-based answers
The risk of a fibroid becoming a uterine sarcoma is extremely low, approximately 0.1%-0.5% (about 1 sarcoma per 6,000 fibroids). Growing fibroids after menopause warrant attention. LDH3 isoenzyme testing and dynamic contrast-enhanced MRI can help differentiate.
No. No international guideline has ever listed fibroid size >5cm as a surgical indication. Surgical indications are based on symptoms: anemia from heavy bleeding, severe pressure symptoms, or fertility impact. Asymptomatic fibroids can be observed and will naturally shrink after menopause.
The timing depends on the surgical approach and fibroid location. Not all cases require a 2-year wait. After laparoscopic or open myomectomy, 1-2 years of contraception is generally recommended. Recovery after hysteroscopic surgery is faster. Discuss your individual situation with your doctor.
Research shows vitamin D deficiency is associated with a 32% increased risk of fibroids — supplementation is recommended. EGCG in green tea has shown some inhibitory effects on fibroids in studies. A balanced diet, regular exercise, and healthy weight maintenance support overall health, but no food can replace medical treatment.
It depends on the location and size. Submucosal and large intramural fibroids may affect conception or increase miscarriage risk. However, many women with fibroids conceive and deliver normally. If planning pregnancy, consult a specialist for evaluation in advance.
Fibroid degeneration refers to degenerative changes within the fibroid, including hyaline, cystic, and red degeneration. Fibroid degeneration is nothing to worry about — it is a benign natural process, not malignant transformation.
Ablation therapy includes HIFU, microwave ablation, and radiofrequency ablation, using thermal energy to cause fibroid tissue necrosis, absorption, and shrinkage. This 'ultra-minimally invasive treatment' offers minimal trauma, fast recovery, with only tiny marks on the abdominal wall.
Fibroids are hormone-dependent. After menopause, most fibroids gradually shrink due to declining estrogen levels. However, if fibroids continue to grow after menopause, uterine sarcoma should be considered, and prompt medical evaluation is recommended.